|
Not all tests are authorized, cleared, or approved by the FDA. Tests must be authorized, cleared, or approved by Members can be reimbursed for up to eight tests per month. HMSA will continue to reimburse Fed 87 members for the price of the tests, including shipping and sales tax, up to $12 per test for 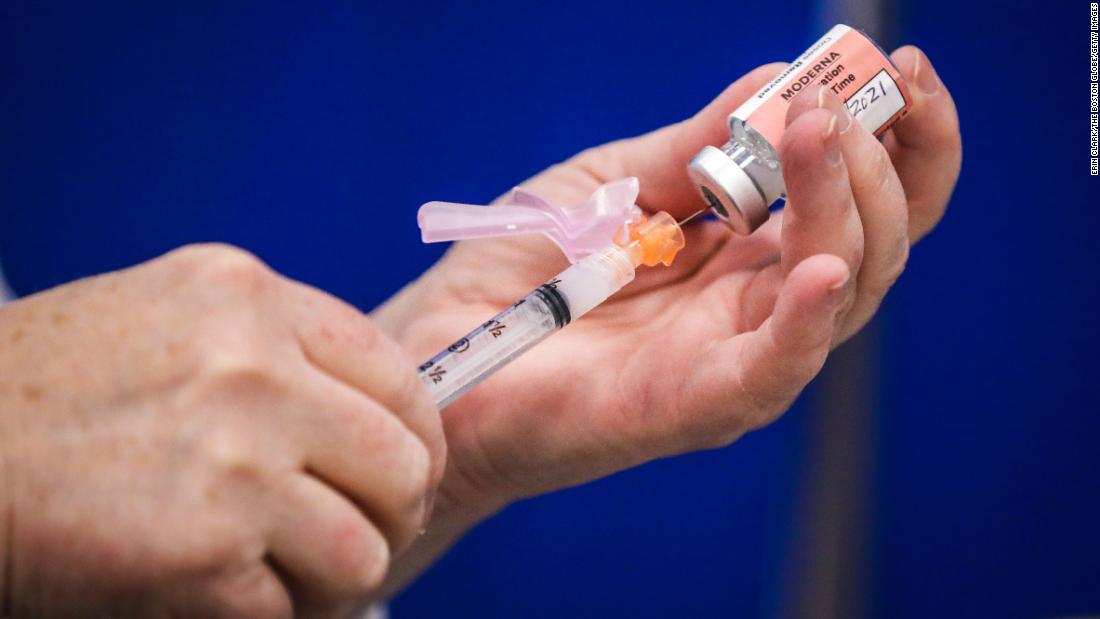
Of ordering through HMSA’s preferred provider, Hawaii Family Medical Center (dba Kuhio Medical Center, a subsidiary of HMSA. Starting May 12, 2023, HMSA will no longer offer commercial plan members OTC at-home tests at no cost. Requestįor reimbursement must be submitted within one year from the date of purchase. Self-insured members who purchased these test kits before May 12, 2023, may request reimbursement through My Account on. HMSA will no longer reimburse costs for over-the-counter COVID-19 test kits purchased on or after May 12, 2023. As a result, the following changes will take effect starting May 12, 2023. Department of Health and Human Services announced that the federal public health emergency for COVID-19 will expire at the end of theĭay on May 11, 2023. HMSA Kaimana Awards & Scholarships Program More MoreĪrticle: KB00341 Important Update Effective May 12, 2023:.Health and Well-being Support More More.Our representativesĬan help you learn about your bill, make payments, check on a claim, explore well-being resources, or start a new plan. For members who use the delivery/shipping service offered by pharmacies in the Direct Coverage network, members will be responsible for delivery or shipping costs, if the pharmacy requires a fee for that service.Take control of your health care by getting answers to your questions from someone who knows.Should members reach that quantity limit based on the claims adjudicated at the pharmacy, any submitted receipts for tests purchased within that same rolling 30-day period will not be reimbursed. Members will only be reimbursed for up to two tests per consecutive 30 days.Members must follow the post-service reimbursement process to receive this reimbursement. A maximum amount of $12 per test will be reimbursed to members who do not obtain the test through Direct Coverage.Circumstances in which costs could be incurred for OTC Covid-19 tests: *In CA tests may be reimbursable subject to additional state law and guidance, as applicable. Your tests must be for personal diagnostic use, have not been and will not be reimbursed by another source, and have not been and will not be for resale. COVID-19 tests for employment or back-to-school purposes are not reimbursable under the federal CARES Act.* Reimbursement guidelines: FDA Authorized OTC COVID self-tests will be reimbursed and include the following. Learn more by visiting our at home COVID reimbursement page here! Also, ideally, your receipt should only include the purchase of tests and no other items. This quantity limit applies to over-the-counter tests without a prescription. Test kits that contain two tests per kit are counted as two tests. Each test is counted separately, even if multiple tests are sold in a single package. 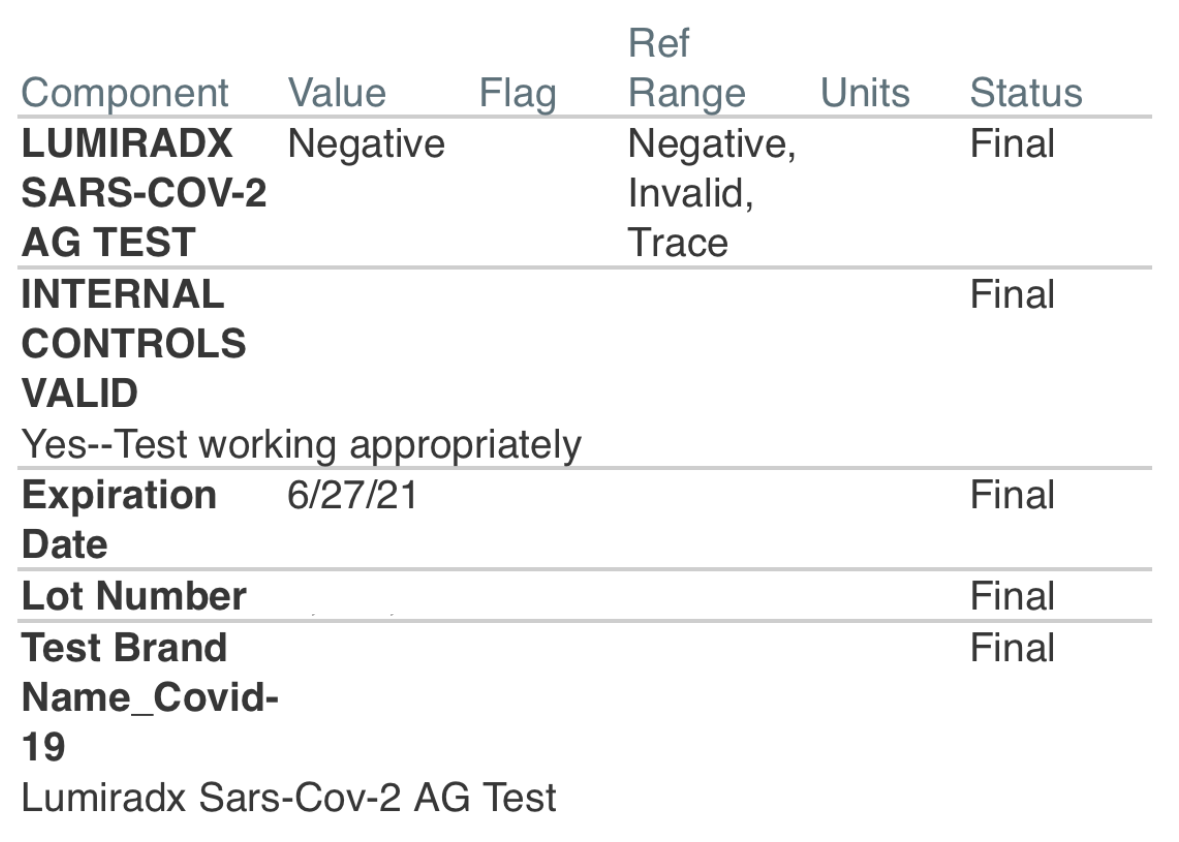
In addition, we’ll only reimburse up to two over-the-counter tests, per individual covered under your plan, per 30 consecutive days 1. You must be an active member enrolled in individually purchased health care or on a small group plan or Medicare Advantage plan. Your tests must be purchased on or after January 15, 2022. In order to reimburse you for a COVID-19 at-home test, here’s what needs to happen: What are the requirements for reimbursement? If you purchase an over-the-counter COVID-19 test from an in-network location and are charged for your test, keep your receipt and submit a claim to us for reimbursement.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
